Three months ago, I couldn’t finish a sentence without losing my train of thought. I’d walk into rooms and forget why. My brain felt wrapped in cotton—thick, slow, unreachable. Doctors ran tests. Thyroid? Normal. Vitamin levels? Fine. Sleep tracker? Seven hours every night.
Let me show you how this happens—and more importantly, how to fix it.
The Gut-Brain Axis: Your Second Brain Is Running the Show
The Communication Highway You Didn’t Know Existed
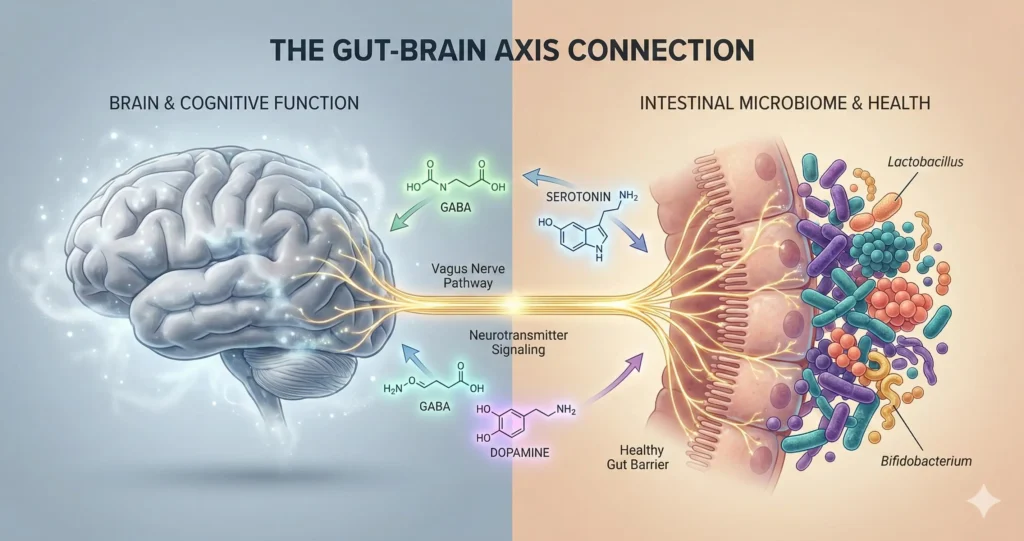
Your gut contains approximately 100 to 500 million neurons—more than your spinal cord. This “second brain,” called the enteric nervous system, doesn’t just digest food. It’s in bidirectional communication with your central nervous system through the gut-brain axis, involving the endocrine, nervous, and immune systems .
Think of it like this: your gut microbiome is a pharmaceutical factory producing compounds that directly influence brain chemistry. When this factory is operating smoothly, you feel sharp, balanced, energized. When it’s compromised, the effects ripple upward—into your mood, cognition, and mental stamina.
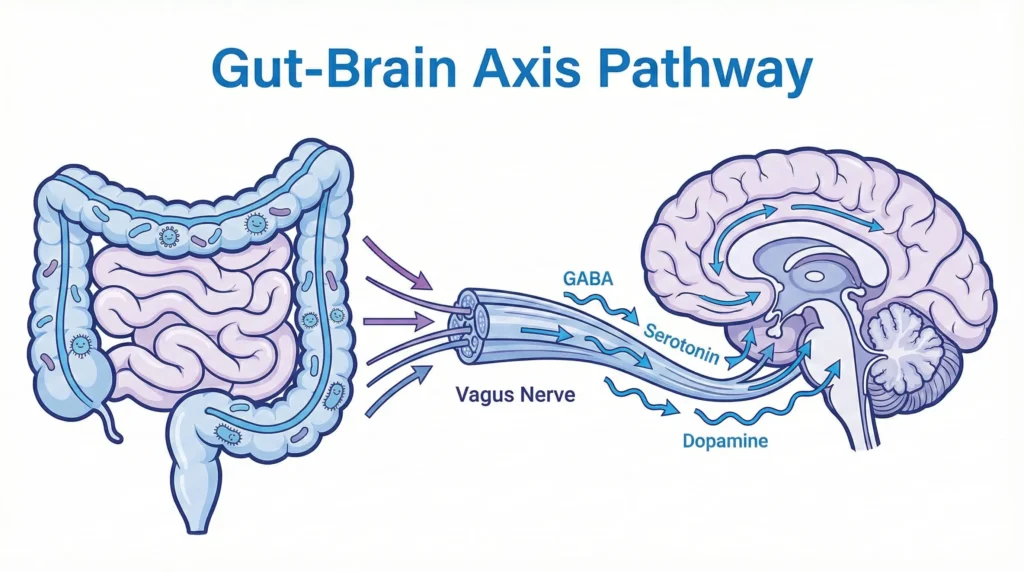
The Three Primary Pathways:
- Vagus Nerve Signaling: The vagus nerve acts as a fiber-optic cable carrying signals from your gut directly to your brainstem. Afferent vagus nerve fibers transport signals from the gastrointestinal tract and gut microbiota to the brain , influencing everything from heart rate to emotional regulation.
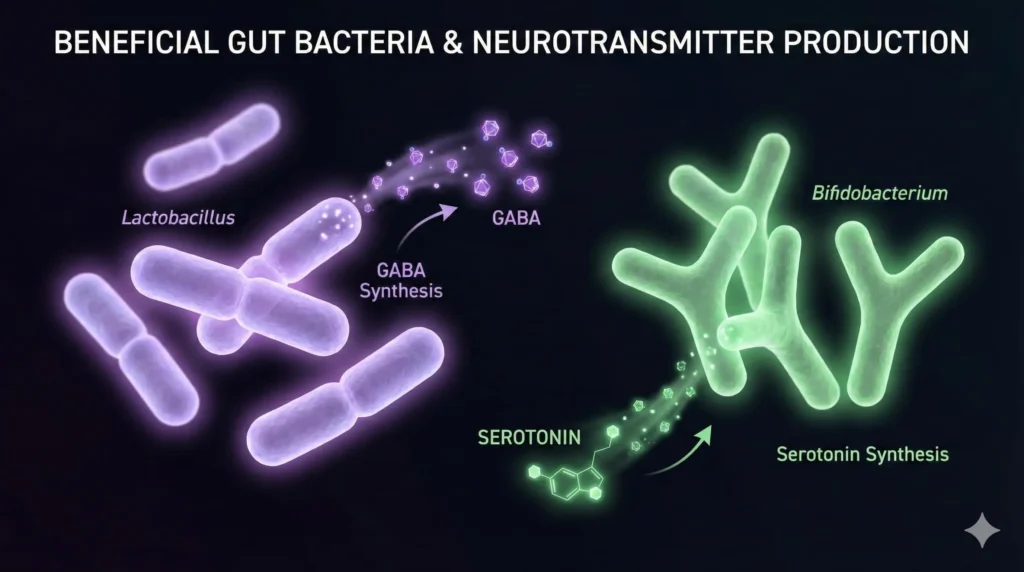
- Neurotransmitter Production: Your gut bacteria synthesize GABA (calming), serotonin (mood regulation), and dopamine (motivation). These don’t need to cross the blood-brain barrier to affect your mental state—they work through the vagus nerve and immune signaling.
- Immune Activation: Approximately 70% of immune cells reside in the gut . When gut permeability increases (leaky gut), inflammatory cytokines enter circulation and reach the brain, triggering neuroinflammation—the root cause of brain fog.
This is why you can’t just “think your way” out of brain fog. If your gut microbiome is dysregulated, your brain is receiving distorted signals—like trying to have a conversation through a staticky phone line.
Dysbiosis: When Your Microbiome Turns Against You
The Hidden Epidemic Destroying Mental Clarity
Dysbiosis is an imbalance in gut bacteria—too many pathogenic species, too few beneficial ones. Intestinal dysbiosis negatively influences gut physiology, causing inappropriate transmission of stimuli along the gut-brain axis and breaking down intestinal permeability .
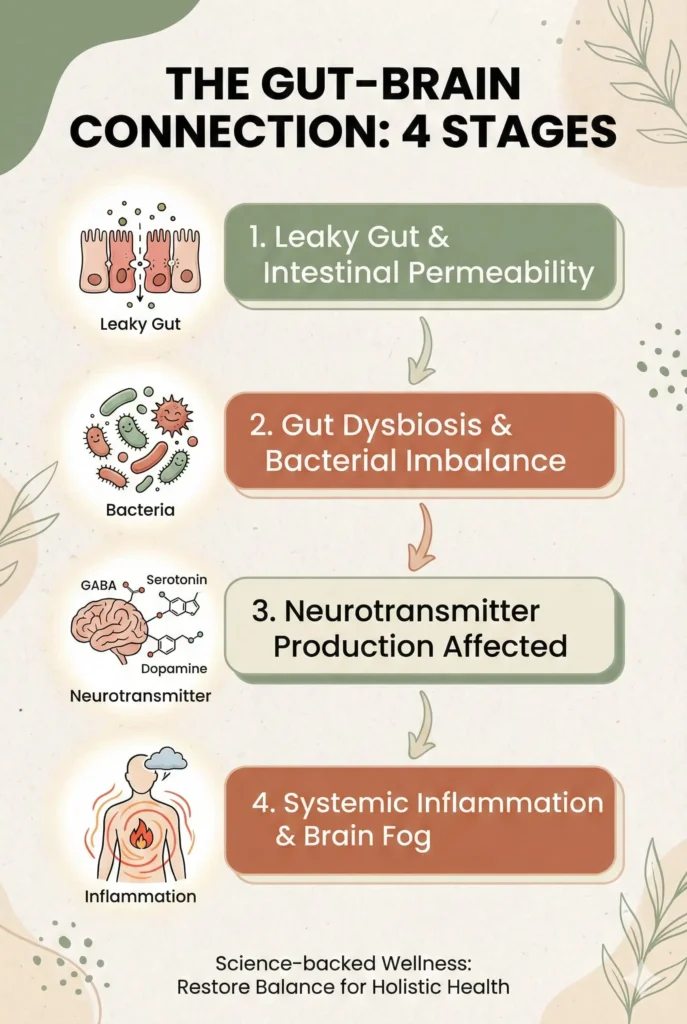
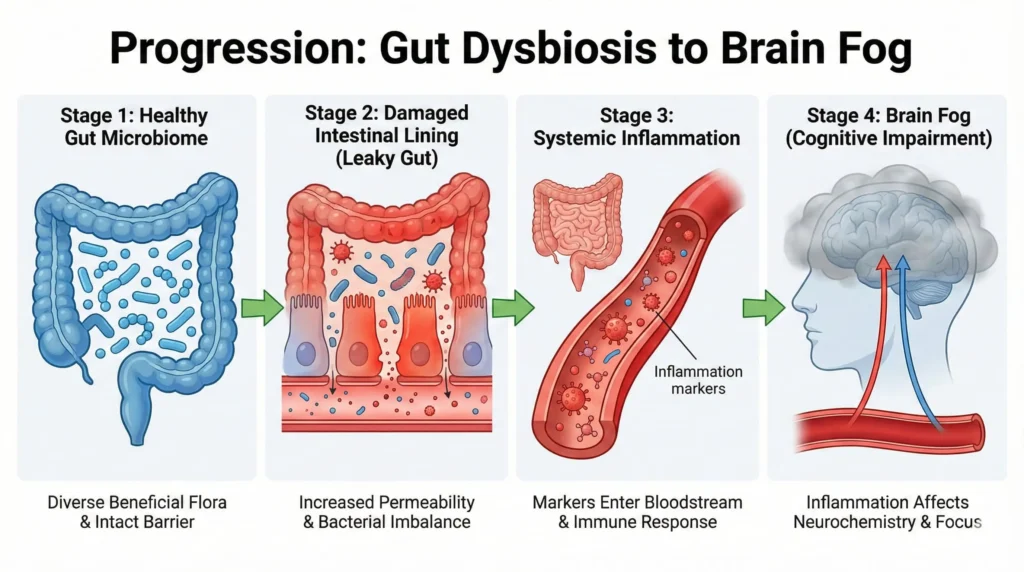
Here’s how it unfolds:
Stage 1: The Trigger
Antibiotics, chronic stress, processed foods, or environmental toxins wipe out beneficial bacteria. Your microbiome diversity plummets. The protective bacterial species that manufacture GABA and regulate inflammation disappear.
Stage 2: Leaky Gut
Without adequate beneficial bacteria, the intestinal lining becomes permeable. An inflamed gut leaks toxins into the bloodstream, strongly impacting cognitive function through brain fog, memory issues, and learning difficulties . Your immune system goes into overdrive, flooding your body with inflammatory cytokines.
Stage 3: Neurotransmitter Disruption
People with IBS and depression have lower levels of gut bacteria involved in making GABA . Without sufficient GABA-producing bacteria like Lactobacillus and Bifidobacterium species, your brain loses its primary calming neurotransmitter. Result? Anxiety, racing thoughts, and an inability to “turn off” your mind.
Stage 4: The Cascade
Gut issues negatively affect dopamine and serotonin production, essential neurotransmitters impacting every aspect of mental health . You experience the full constellation of symptoms: brain fog, mood swings, poor concentration, fatigue, and unexplained anxiety.
I lived in Stage 4 for two years before I understood what was happening. Once I started addressing gut health through targeted interventions (more on this below), my brain fog lifted within three weeks. Not gradually—dramatically.
The GABA Crisis: Your Gut’s Calming Chemical Is Missing
Why You Can’t Calm Your Mind
GABA (gamma-aminobutyric acid) is your brain’s primary inhibitory neurotransmitter. It’s what allows you to relax, focus, and sleep deeply. Imbalances in neurotransmitters including GABA are associated with cognitive impairment .
Here’s the breakthrough: Gut microbes produce GABA through the glutamate decarboxylase system, with key enzyme GAD converting glutamate to GABA . Specific bacterial genera—particularly Bacteroides, Lactobacillus, and Bifidobacterium—are your gut’s GABA factories.
What Kills GABA Production:
- Antibiotic use (even months later, the damage persists)
- High-sugar diets (feed pathogenic bacteria, starve beneficial ones)
- Chronic stress (elevates cortisol, which alters microbiome composition)
- Artificial sweeteners (disrupt bacterial balance)
- Insufficient fiber (GABA-producing bacteria need prebiotics to thrive)
Research shows GABA produced by gut microbiota may affect host behavioral characteristics via GABA receptors in intestinal epithelial cells —meaning you don’t even need it to reach your brain for it to work. The gut-to-brain signaling happens through the vagus nerve and immune pathways.
This is where targeted supplementation becomes critical. While I focus on food-first approaches (fermented foods, prebiotic fiber), I also use Brain Song to support this pathway. It’s a nootropic formula specifically designed with adaptogens and compounds that help buffer the stress response and support neurotransmitter balance—essentially giving your gut-brain axis the raw materials it needs while you’re rebuilding your microbiome.
Serotonin: The Mood Regulator Your Gut Controls
Why 90% of Your “Happy Hormone” Lives in Your Gut
Most people think serotonin is made in the brain. Wrong. Approximately 90% of your body’s serotonin is produced in your gut, specifically in enterochromaffin cells that line your intestinal wall.
Gut bacteria alter host serotonin levels by secreting molecules like short-chain fatty acids that signal enterochromaffin cells to produce serotonin . Your microbiome doesn’t manufacture serotonin directly—it orchestrates its production through metabolic signaling.
The Kynurenine Pathway Problem:
When your gut is inflamed, tryptophan (serotonin’s precursor) gets shunted into the kynurenine pathway instead of serotonin production. The entrance of gut tryptophan into the immune-driven kynurenine pathway may play a major role in serotonin dysregulation . This produces neurotoxic metabolites instead of mood-stabilizing serotonin.
Translation? Chronic gut inflammation literally reroutes the biochemical pathway that should be making you feel good—and converts it into one that makes you feel anxious and mentally sluggish.
How to Restore Serotonin Production:
- Reduce gut inflammation (eliminate processed foods, increase omega-3s)
- Consume tryptophan-rich foods (pasture-raised turkey, wild-caught fish, pumpkin seeds)
- Support spore-forming bacteria through fermented foods
- Prioritize simple morning habits that reduce cortisol and support circadian rhythm
The Stress-Gut-Brain Cycle: Breaking the Feedback Loop
Why Stress Makes Everything Worse
The gut-brain axis is highly sensitive to stress, with cortisol altering gut motility, increasing intestinal permeability, and shifting the microbiome toward a pro-inflammatory state .
This creates a vicious cycle:
- Stress elevates cortisol → Damages gut lining
- Damaged gut → Inflammatory cytokines enter bloodstream
- Inflammation reaches brain → Triggers more stress response
- More cortisol → Further gut damage
Psychological stress impacts gut microbiome makeup, either through diet changes or direct molecular signals from brain to gut . This is why you can’t just “manage stress” with meditation alone if your gut is compromised—you need to address both ends of the axis simultaneously.
Breaking the Cycle:
- Morning sunlight exposure: Start with a 5-minute morning ritual that includes direct sunlight. This regulates cortisol timing and supports circadian rhythm.
- Vagus nerve activation: Deep breathing, humming, and gargling stimulate vagal tone. Breathwork techniques activate the parasympathetic response, reducing gut-related anxiety .
- Magnesium supplementation: 400mg glycinate before bed supports GABA receptor function and reduces stress-induced gut permeability.
- Strategic movement: Incorporate simple morning stretches to activate the vagus nerve and improve gut motility.
The Keto-Gut-Brain Connection: Why Low-Carb Works
How Metabolic Flexibility Heals the Gut-Brain Axis
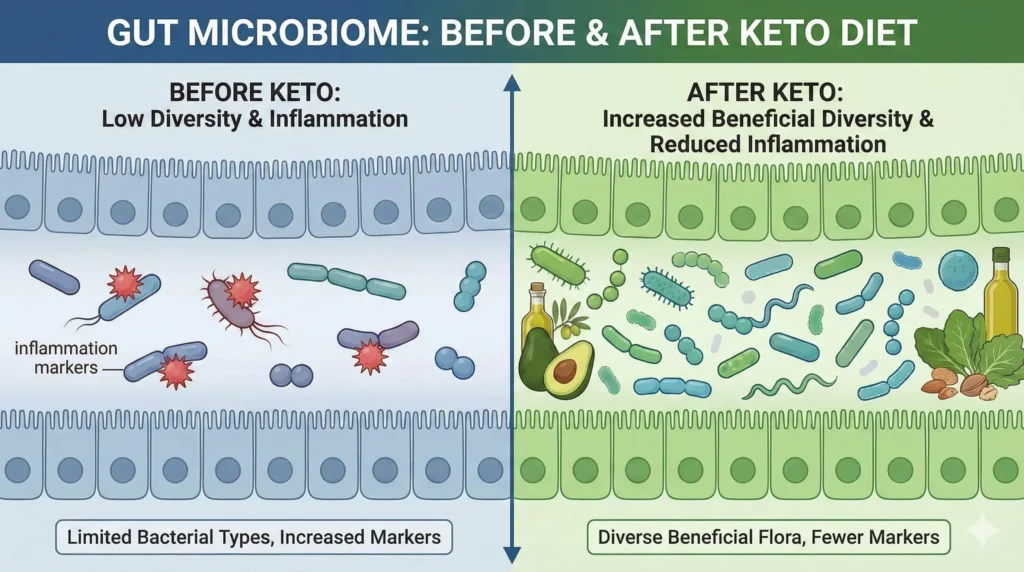
When I transitioned to a ketogenic approach, my brain fog improved faster than with any other intervention. Here’s why: blood sugar volatility is one of the primary drivers of gut inflammation and microbiome disruption.
High-carb diets feed pathogenic bacteria (like Candida and harmful Proteobacteria) while starving beneficial species. The result? Endotoxin production, increased intestinal permeability, and systemic inflammation that directly impairs cognitive function.
Keto’s Gut-Brain Benefits:
- Reduced inflammation: Ketones (especially beta-hydroxybutyrate) have direct anti-inflammatory effects on gut lining
- Stable neurotransmitter production: No blood sugar crashes means consistent GABA and serotonin signaling
- Improved microbiome diversity: Healthy fats and fiber feed beneficial bacteria
- Enhanced mitochondrial function: Better cellular energy in both gut and brain tissue
If you’re new to this approach, start with simple keto habits for wellness rather than jumping into strict macros. Focus on eliminating processed carbs, increasing healthy fats, and eating within a consistent window.
Pair this with support for mental clarity and metabolic function. I personally use Brain Song during my transition into ketosis because it contains adaptogens that help smooth out the “keto flu” phase while supporting the cognitive benefits. The formula works synergistically with a low-carb approach to enhance both gut healing and mental performance.
The 4-Week Gut-Brain Reset Protocol
Practical Steps to Restore Mental Clarity
This isn’t theory—it’s the exact protocol I used to eliminate my brain fog. Results started appearing within 10 days, with full clarity restored by week four.
Week 1: Elimination Phase
- Remove all processed foods, refined carbs, and vegetable oils
- Eliminate artificial sweeteners (they devastate microbiome diversity)
- Cut out alcohol completely (it increases intestinal permeability)
- Begin mindful eating habits to improve digestion and reduce stress while eating
Week 2: Rebuilding Phase
- Introduce fermented foods daily: sauerkraut, kimchi, full-fat yogurt, kefir
- Increase prebiotic fiber: asparagus, garlic, onions, Jerusalem artichokes
- Add bone broth (collagen repairs intestinal lining)
- Supplement with high-quality probiotics containing Lactobacillus and Bifidobacterium strains
Week 3: Optimization Phase
- Implement time-restricted eating (12-hour window minimum)
- Increase omega-3 intake: wild-caught fatty fish 3-4x weekly
- Add polyphenol-rich foods: berries, dark chocolate, green tea
- Prioritize evening habits for better sleep (gut repair happens during deep sleep)
Week 4: Maintenance Phase
- Continue fermented foods and prebiotic fiber
- Add targeted supplements: magnesium glycinate, omega-3s, vitamin D3
- Practice daily vagus nerve activation (deep breathing, cold exposure)
- Monitor mental clarity and adjust based on response
The Long COVID Connection: Why Brain Fog Persists
Post-Viral Dysbiosis and Neuroinflammation
Brain fog and cognitive dysfunction are common psychological manifestations of post-acute COVID infection . The mechanism? Persistent gut dysbiosis that continues long after viral clearance.
Observational evidence reveals gut microbiome compositional changes in patients with PASC, including decreased abundance of beneficial butyrate producers . Butyrate is a short-chain fatty acid that repairs the gut lining and reduces neuroinflammation.
If you’re experiencing post-viral brain fog, the gut-brain axis approach is even more critical. The virus disrupts microbiome balance, and that disruption perpetuates cognitive symptoms months or years later—even when the virus is gone.

Testing and Tracking: Know Your Microbiome
Data-Driven Gut Health Optimization
You can’t manage what you don’t measure. Consider comprehensive stool testing through companies like Thorne, Viome, or Doctor’s Data to identify:
- Bacterial diversity and abundance
- Pathogenic overgrowth (Candida, Klebsiella, etc.)
- Inflammatory markers (calprotectin)
- Digestive function (elastase, fat absorption)
- SCFA production levels
Subjective Tracking Metrics:
- Morning mental clarity (rate 1-10 upon waking)
- Sustained focus duration (how long can you work without brain fog?)
- Mood stability throughout the day
- Digestive symptoms (bloating, regularity)
- Sleep quality (especially deep sleep percentages)
FAQ: Your Gut-Brain Questions Answered
How long does it take to heal gut dysbiosis and brain fog?
Most people notice initial improvements within 7-14 days of implementing dietary changes and probiotic support. Full restoration of microbiome diversity typically takes 8-12 weeks, with cognitive improvements appearing progressively throughout this period. Severe dysbiosis may require 6-12 months of consistent intervention.
Can I fix brain fog without changing my diet?
Unlikely. While supplements and lifestyle modifications help, diet is the primary driver of microbiome composition. Your gut bacteria are literally made from what you eat. Processed foods and refined carbs feed pathogenic species, while whole foods and fiber support beneficial bacteria. There’s no way around this fundamental biochemical reality.
Do I need antibiotics if I have gut dysbiosis?
Only in cases of documented SIBO (small intestinal bacterial overgrowth) or specific pathogenic infections. For general dysbiosis, antibiotics often worsen the problem by killing beneficial bacteria alongside harmful ones. Focus on crowding out bad bacteria with beneficial species through fermented foods, prebiotics, and lifestyle modification first.
What’s the best probiotic for brain fog?
Look for multi-strain formulas containing Lactobacillus plantarum, Lactobacillus brevis, Bifidobacterium longum, and Bifidobacterium adolescentis. Lactobacillus brevis has been shown to produce the highest levels of GABA . Rotate probiotic strains every 2-3 months to maximize diversity.
Can keto hurt my gut microbiome?
Only if done incorrectly. A poorly formulated ketogenic diet lacking fiber and vegetables can reduce beneficial bacteria. However, a well-designed keto approach rich in non-starchy vegetables, fermented foods, and healthy fats actually improves microbiome diversity and reduces inflammation. Focus on nutrient density, not just macro ratios.
How do I know if my brain fog is gut-related vs. something else?
Gut-related brain fog typically includes concurrent digestive symptoms (bloating, irregular bowel movements, food sensitivities), worsens after meals high in sugar or processed foods, and improves with fasting or gut-supportive interventions. If you have no digestive symptoms, investigate other causes like thyroid dysfunction, sleep apnea, or chronic infections. That said, gut issues can exist without obvious digestive symptoms —neurological manifestations sometimes appear first.
The Bottom Line: Your Brain Is Only As Healthy As Your Gut
Three years ago, I thought brain fog was just part of aging, stress, or “having a lot on my mind.” I tried everything: nootropics, meditation apps, sleep optimization, therapy. Nothing worked until I addressed the root cause—my gut microbiome.
The science is unequivocal: the gut microbiota influences CNS function through the production of hormones, immune factors, and metabolites like short-chain fatty acids . Your mental clarity isn’t determined solely by what’s happening in your skull—it’s shaped by the trillions of bacteria in your digestive tract.
The gut-brain axis isn’t pseudoscience or wellness marketing. It’s fundamental human physiology. And once you understand how to optimize it, you gain access to cognitive performance you didn’t know was possible.
Start with the 4-week protocol. Track your results. Give your microbiome the support it needs through targeted nutrition, strategic supplementation, and lifestyle modifications that reduce stress and inflammation.
Your brain fog isn’t a life sentence. It’s a symptom of a system that can be repaired—one meal, one habit, one bacterial colony at a time.

Elena Hartwell is a wellness educator specializing in sleep optimization, metabolic health, and natural weight management. After years of struggling with exhaustion and unexplained weight gain despite “doing everything right,” Elena discovered the powerful connection between sleep quality, gut health, and metabolism—a breakthrough that transformed her life and inspired her mission. Today, she translates cutting-edge research into simple, actionable strategies that help readers sleep better, lose stubborn weight naturally, and reclaim their energy. Elena’s evidence-based approach has helped thousands break free from the diet-exercise cycle by addressing the root cause: disrupted sleep and metabolic dysfunction.